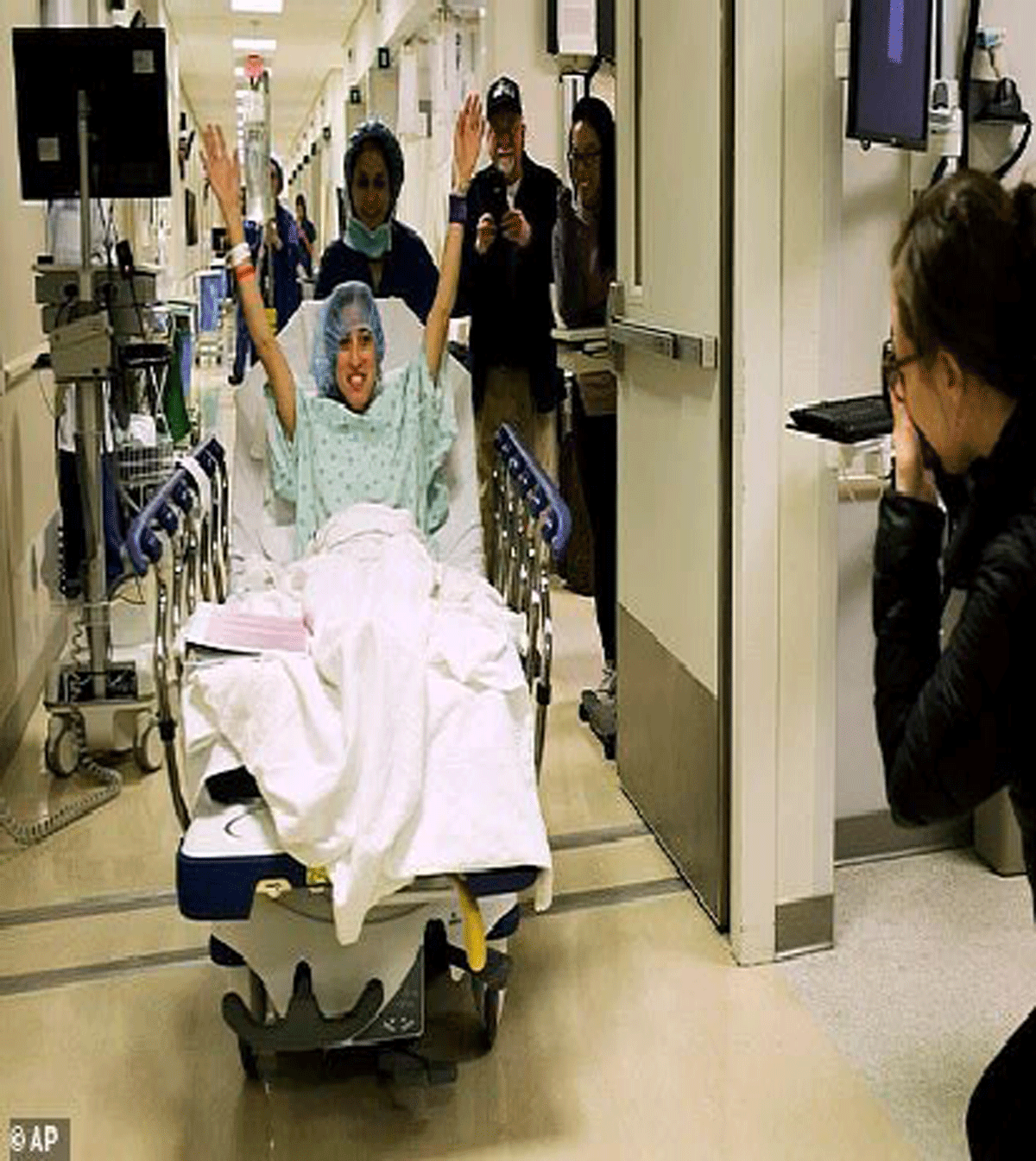
•Nina Martinez, 35, (pictured) got HIV from a blood transfusion at six weeks old in 1983 before blood banks screened for HIV. Fortunately, she lived to 13, when viral-suppressing drugs were released. She has donated a kidney in a world first
By Sola Ogundipe
Surgeons in Baltimore have performed what’s thought to be the world’s first kidney transplant from a living donor with HIV, a milestone for patients with the AIDS virus who need a new organ.

•Nina Martinez, 35, (pictured) got HIV from a blood transfusion at six weeks old in 1983 before blood banks screened for HIV. Fortunately, she lived to 13, when viral-suppressing drugs were released. She has donated a kidney in a world first
If other donors with HIV come forward, it could free up space on the transplant waiting list for everyone.
Martinez, whose HIV is suppressed by drugs to an undetectable level, first started exploring donation so she could give her kidney to an HIV-positive friend who needed one.
We don’t need foreign agencies to fight HIV, Says Aisha Buhari
Her friend died before tests were through, but Martinez decided to honor him by donating it to a stranger, who is also HIV-positive.
On Monday March 25, she traveled from her home in Atlanta to Johns Hopkins University for the operation.
“Don’t call me a hero, call me the first. I want to see who comes next,’ Martinez said
She told the Associated Press she ‘wanted to make a difference in somebody else’s life’ and counter the stigma that too often still surrounds HIV infection.
Many people think ‘somebody with HIV is supposed to look sick,’ Martinez, 35, told The Associated Press before the operation.
‘It’s a powerful statement to show somebody like myself who’s healthy enough to be a living organ donor.’
Hopkins said both Martinez and the recipient of her kidney, who chose to remain anonymous, are recovering well.
‘Here’s a disease that in the past was a death sentence and now has been so well controlled that it offers people with that disease an opportunity to save somebody else,’ said Dr Dorry Segev, a Hopkins surgeon who pushed for the HIV Organ Policy Equity, or HOPE, Act that lifted a 25-year US ban on transplants between people with HIV.
Surgeons planning world’s first HEAD transplant claim they repaired ‘irreversible’ spinal cord injuries in monkeys and dogs—which they say is proof they can start human trials.
There’s no count of how many HIV-positive patients are among the 113,000 people on the nation’s waiting list for an organ transplant. HIV-positive patients can receive transplants from HIV-negative donors just like anyone else.
Only in the last few years, spurred by some pioneering operations in South Africa, have doctors begun transplanting organs from deceased donors with HIV into patients who also have the virus, organs that once would have been thrown away.
Since 2016, 116 such kidney and liver transplants have been performed in the U.S. as part of a research study, according to the United Network for Organ Sharing, or UNOS, which oversees the transplant system.
One question is whether receiving an organ from someone with a different strain of HIV than their own poses any risks, but so far there have been no safety problems, said UNOS chief medical officer Dr. David Klassen.
Hopkins’ Segev said Monday’s kidney transplant was a world first. Doctors had hesitated to allow people still living with HIV to donate because of concern that their remaining kidney would be at risk of damage from the virus or older medications used to treat it.
But newer anti-HIV medications are safer and more effective, Segev said. His team recently studied the kidney health of 40,000 HIV-positive people and concluded that those with well-controlled HIV and no other kidney-harming ailments like high blood pressure should face the same risks from living donation as someone without HIV.
Martinez, a public health consultant, became interested in living donation even before HIV-to-HIV transplants began. Then last summer she learned that an HIV-positive friend needed a transplant and she started actively pursuing it
‘There are potentially tens of thousands of people living with HIV right now who could be living kidney donors,’ said Segev, who has advised some other hospitals considering the approach.
Generally, kidneys from living donors last longer, added Dr Niraj Desai, the Hopkins surgeon caring for the recipient. And if more people living with HIV wind up donating, it helps more than HIV-positive patients who need a kidney.
‘That’s one less person waiting for a limited resource,’ Desai said. ‘That helps everybody on the list.’
HIV is spread in certain body fluids from a person who has HIV. These fluids are blood, semen, pre-seminal fluids, rectal fluids, vaginal fluids, and breast milk.
HIV is spread mainly by having sex or sharing injection drug equipment, such as needles, with someone who has HIV.
To reduce risk of HIV infection, use of condoms correctly every time during sex is recommended. Don’t inject drugs. If you don’t have HIV, but are at high risk of becoming infected with HIV, talk to your health care provider about pre-exposure prophylaxis (PrEP). PrEP involves taking a specific HIV medicine every day to reduce the risk of HIV infection.
According to the Baltimore Sun, a number of medical breakthroughs have been performed at the Johns Hopkins.
In 2018, a Johns Hopkins surgery team of nine plastic surgeons and two urological surgeons performed the first total penis and scrotum transplant and part of an abdominal wall on a wounded soldier.
The most common procedures are kidney and liver transplants, followed by heart transplants. However, doctors in Baltimore and elsewhere have successfully transplanted other body parts from deceased donors to living candidates.
In 2013, the Hopkins team performed a double arm transplant on Brendan Marrocco, who lost both of his arms, as well as his legs, in the Iraq war when the armoured vehicle he was driving ran over a bomb in 2009.
Jerome Hamon received his first face transplant in 2010, but it needed, to be removed last year after he became ill.
Hamon’s first face was donated by a 60-year-old. With his second transplanted face— from a 22 year-old donor—Hamon, 43, joked that he managed to drop a few decades.
France was also the first country to be site of a face transplant. The procedure has since been performed several times in Baltimore.
In 2012, doctors at the University of Maryland performed the most extensive face transplant at the time on a Virginia man named Richard Lee Norris, who received donor skin from his scalp to his neck, as well as a new jaw, teeth, tongue and the underlying muscle and tissue. In addition to matching his blood type, doctors had to match his skin color and bone structure to a donor.
The University of Maryland has pioneered other transplant surgeries as well. In 2016, doctors at the University of Maryland Medical Centre were able to perform a kidney transplant on a patient with no need for dialysis—a feat they said was the first type of procedure in the country.
World AIDS Day: LAPO screens 100 Artisans in Lagos
Also in 2016, Hopkins doctors performed the nation’s first liver and kidney transplants from a donor infected with HIV to recipients also infected with the virus.
It was a triumph for one of the transplant surgeons, Dorry L. Segev, who fought for six years for federal approval of the life-saving surgery.
In July 2015, an 8-year-old boy from Owings Mills became the first child to receive a bilateral hand transplant. Doctors at Children’s Hospital of Philadelphia meticulously took the hands and forearms from the donor and attached them to the limbs of Zion Harvey, connecting bone, blood vessels, nerves, muscles, tendons and skin.
Some territory remains uncharted in the field of organ transplantation. Italian Dr. Sergio Canavero visited Annapolis in 2015, to speak about his ambition to conduct the world’s first head transplant. The controversial surgeon suggested that, contrary to accepted modern medicine, it’s possible to repair a severed spine. Some weren’t so sure.
“There was not much science in his talk,” said Dr. Dinesh Ranjan, a transplant surgeon from Lexington, Ky. “This is something that may happen, but not by him.”
Disclaimer
Comments expressed here do not reflect the opinions of Vanguard newspapers or any employee thereof.