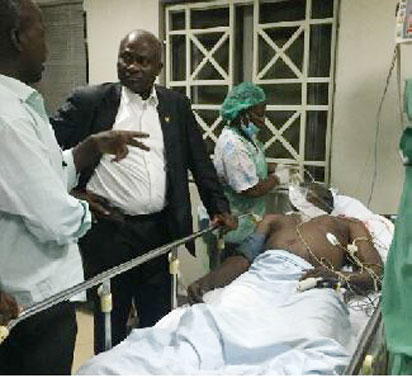
VISIT: The Lagos State Commissioner for Health, Dr. Jide Idris during his visit to fire accident victims at the Lagos University Teaching Hospital, LASUTH.
Says officials indicted in the death of pregnant woman in Alimosho hospital will pay for it
•’How we are moving medical sector forward’
By Chioma Obinna
Access to quality healthcare in Lagos has been the focus of the state government in the last 16 years. Unfortunately, the targets have not been met following many challenges including shortage of medical personnel, migration of patients from neighbouring states and the inability to design and plan for standard hospital facilities.
A third-time Commissioner for Health in the state, Dr Jide Idris, in this encounter, sheds light on his plans to correct the anomalies and strengthen the sector.
He also recounts how the state defeated the dreaded Ebola Virus Diseases (EVD). Excerpts:
Summary of events at the end of last tenure
During the last tenure, our achievements cut across infrastructure, primary healthcare, human resource, healthcare financing, regulation and, of course, health promotion and disease prevention. We started the maternal and child mortality prevention programme, but, in the last six months, the statistics I am seeing, I am not too happy because nothing has happened during that period but it is a priority.
The major one we are going to start now is healthcare promotion and disease prevention, in the sense that we cannot do everything at once. We also have ongoing programmes on malaria control, we are the only state that is doing RRS, apart from insecticide treated net, diagnoses among others.
On infrastructure, we have built so many facilities and have increased the scope of services many times. At the primary care level, there is quite a number of Primary Healthcare Centres, PHCs, that were not functioning. Efforts were made to revitalize the PHC system and we came up with the idea of Flagship PHC for each local government.
But the fact is that there are still PHCs that need to be made functional. That is why we have a huge number of people visiting our secondary facilities and congesting them.
At secondary care level, there were some facilities that we needed to increase their scope of services to make them General Hospitals. We tried a couple and built Maternal and Child Centres (MCCs) to complement services in some of the General Hospitals. We built seven out of the 10 we planned, and the remaining three are at different levels of completion. We have refurbished some hospitals too but there are still a lot of things to do.
Plans for hospital facilities
What is being planned for this session is to continue what has been done. However, there is the need to address some specific issues. Luckily, the governor, even before he constituted his cabinet, had earmarked some hospitals for renovation and to increase their scope. If you look at it over the years, none of our hospitals was purposely built as a General Hospital. So, in this case, if we are to do anything in that line, we must do it properly. So, we are reviewing the situation.
For instance, the plan now is to knock down some of these buildings and put things that will make their functioning complete. Alimosho will have a full-fledged outpatient services. Epe too is going to be addressed and same for Ifako-Ijaye, where we had issues getting the NYSC, mosques among others out of the premises.
LASUTH is overwhelmed and we have told them to stop putting more structures there. Whatever tertiary service is needed, let us expand to other places. That is why we have the Cardiac and Renal Centre and also Trauma and Burn Centre in Gbagada. Whatever else is needed should be sited in other General Hospitals to decentralise.
Addressing shortage of health workers

FILE: The Lagos State Commissioner for Health, Dr. Jide Idris during his visit to fire accident victims at the Lagos University Teaching Hospital, LASUTH.
Obviously, there is gross shortage of workforce. People say we have the highest health workforce but that is not enough. We have about 1,800 doctors and over 5,000 nurses to over 20 million population. We are victims of our own successes. More people are coming into Lagos and that is compounding the problem. People come from other states to use our facilities and we cannot drive them away. About three years ago when we did our statistics, about 25 per cent of patients in our facilities come from outside of the state. I think they are more now.
A major challenge concerning human resources is inter-professional rivalry among the stakeholders in the health sector. Though it is not peculiar to Lagos, we need to address that, otherwise it will affect service delivery. We will sit with them to address their issues that are often not unconnected with welfare, remuneration and workload among others.
There is also the issue of quality of service vis-à-vis the capacity on ground. There are some specialties that we need in numbers because we have them in acute shortage. For instance, radiographers, radiologists and anaesthetists are in acute shortage nationally. Generally, most of them don’t like to be employed because they prefer to moonlight, but it doesn’t augur well for government. Along that line, we decided to train nurse-anaesthetists at the diploma level and that training will continue.
Effects of shortage on services
We need to find out the causes of poor attitudes to address them. Some of them have to do with welfare, workload and some of them are personal (self interest). In the light of what happened in the last couple of weeks, we have seen some staffers not behaving normally and we are ready to increase the rate of monitoring to check them.
In the last three weeks, I have been to three hospitals and what I discovered was amazing. There are management issues. It was in that process that I sent the State Health Facility Monitoring and Accreditation Agency (HEFAMA) out to General Hospitals. Emerging from that is that I have given three Medical Directors (MDs) one week ultimatum to correct the problems they have. It is very likely that I will have to move some of them around. I think they are human issues that we can solve. Take for instance the problem at Aregbesola PHC in Alimosho (where a woman in labour was allegedly abandoned to die). I have summoned all of them who had connection with the deceased patient and have served them query to explain their roles. The stories I was hearing were conflicting. I also called the husband and he came here to tell his own side of the story, which was very revealing. I have since set up a committee to look into the matter and we are expecting their report. In addition to that now, there is zero tolerance for MDs who don’t perform because they are the people that are supposed to represent us in the local governments. There are other ways I’m using people to get information about the facilities.
Bed space syndrome at LASUTH
LASUTH was built as a Cottage Hospital, from which it rose to district, then General Hospital and we now turned it into Teaching Hospital. It was a 400-bed facility when it started. It is now 750-bed and still grossly inadequate. As a Teaching Hospital, it cannot function effectively because, in a Teaching Hospital, you cannot have roads in-between and start wheeling patients to the theatre.
Initially, we planned to knock down that place and build another one somewhere in Matori but the cost is huge. And if you build it, you must have adequate staff. That is why we decided to refurbish that place to serve us for now.
Health insurance
Healthcare financing is related to some of the things that we are facing here and it is not unrelated to the demand for universal health coverage. We can increase physical access by building facilities, but without staff they become useless. Luckily, we have the health insurance bill that was passed last June, but unfortunately we had the 2015 general elections and the change of government. What I have done now is to set up a committee to look at the production of a guideline based on the law, to operate the health insurance scheme. They have started the work but it is complex. Luckily, we have the IFC to support and also PATHS2 and USAID.
Any health system that doesn’t have a financing complement will not work. Health insurance is compulsory in those countries where they are operating it. In our law, it is contributory and, within that law also, there are specifics for the poor that will be addressed and paid for by government. The idea is that if we do it properly, we also stand to benefit from the National Health Act when it begins to function, especially in the area of maternal and child health.
Along that line again, we are trying to push for increased budget for health. From what was shown to us in the current budget, there is increased allocation of about eight per cent, though a huge chunk of that is going into personnel. We still have a huge personnel shortage because of our population.
Disclaimer
Comments expressed here do not reflect the opinions of Vanguard newspapers or any employee thereof.